Inquiries on the study
Takashi Kumada
Visiting Professor, Graduate School of Biomedical and Health Sciences, Hiroshima University
Specially Appointed Professor, Faculty of Nursing, Gifu Kyoritsu University
Email: takashi.kumada * gmail.com
(Note: Please replace * with @)
Inquiries on the story
Hiroshima University Public Relations Office
E-mail: koho * office.hiroshima-u.ac.jp
(Note: Please replace * with @)
Researchers at Hiroshima University and Gifu Kyoritsu University identified Hepatitis B RNA serum levels as a biomarker that more accurately stratifies risk of liver cancer in individuals who have been functionally cured of chronic hepatitis B.
(Point Normal / Unsplash)
Chronic hepatitis B is a viral disease that affects the liver and greatly increases the risks of liver cirrhosis and hepatocellular cancer (HCC, liver cancer). It affects approximately 296 million people worldwide. Hepatitis B is treatable; with the advent of nucleoside (nucleotide) analog (NA) therapy, viral replication is suppressed, reducing the risk of disease progression.
NA therapy results in partial cures (undetectable viral DNA but detectable viral antigen levels) in most cases, and, rarely, functional cures (undetectable viral DNA and antigen levels). However, due to the biology of the hepatitis B virus, the development of HCC cannot completely be prevented, even in the rare cases of functional cures.
Researchers at Gifu Kyoritsu University and Hiroshima University examined the use of novel biomarkers to accurately determine HCC risk. Specifically, they showed that hepatitis B viral RNA (HBV RNA) is better for this purpose compared to both currently used biomarkers as well as other proposed biomarkers.
Their findings were published in the journal Alimentary Pharmacology & Therapeutics on December 2, 2025.
"The introduction of NA medications has dramatically improved outcomes for patients with chronic hepatitis B,” says Takashi Kumada, specially appointed professor, Gifu Kyoritsu University; visiting professor, Graduate School of Biomedical and Health Sciences, Hiroshima University; and first and corresponding author of the study. “However, because HBV is a DNA virus that integrates into the host genome, a complete cure is not achievable. As a result, we cannot completely prevent the development of hepatocellular carcinoma (HCC). Hence, there has been a strong need for reliable biomarkers to accurately predict HCC occurrence in these patients.”
The researchers conducted a retrospective study of chronic hepatitis B patients who had visited Ogaki Municipal Hospital between December 2000 and May 2024 for NA therapy. Of 857 patients, 311 patients met all the prerequisites for inclusion in the study. The predominant HBV genotype was C, accounting for 88.5% of the cases.
With written informed consent, the researchers compiled the medical records of these 311 patients, including NA therapy, serum hepatitis B surface antigen (HBsAg), and serum HBV DNA records. They also analyzed stored serum samples from the patients for novel HBV markers identified in more recent research: HBV core-related antigen (HBcrAg) and HBV RNA.
The 311 patients achieved undetectable HBV DNA levels on NA therapy. Of these, 132 patients had quantifiable HBV RNA levels, and 229 had quantifiable HBcrAg levels. Thirty-one patients developed HCC over the follow-up period, with a median time of 7.8 years.
“Our study demonstrates for the first time that among patients with undetectable HBV DNA, those who test positive for serum HBV RNA have a significantly higher risk of developing HCC. We found that HBV RNA shows better predictive performance than HBcrAg,” Kumada said.
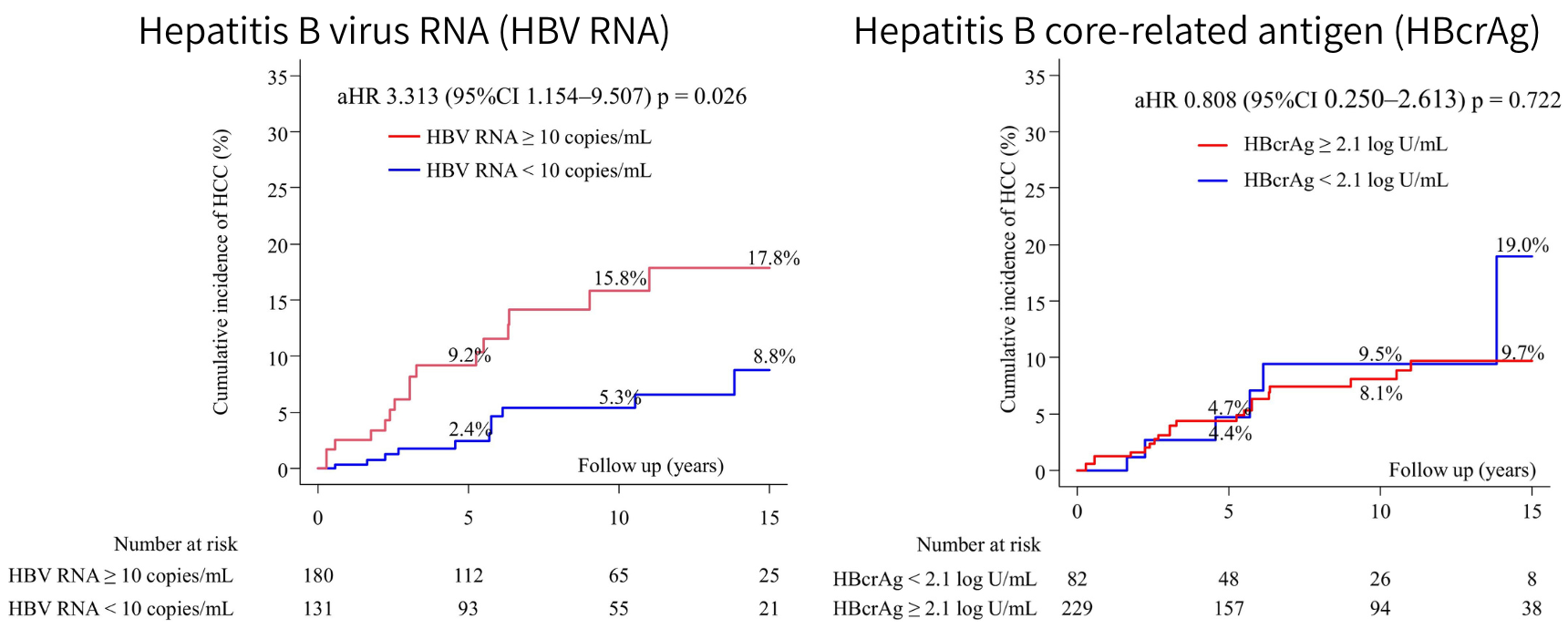
Hepatitis B virus RNA (HBV RNS) predicts hepatocellular carcinoma (HCC) despite viral suppression. Serum HBV RNA levels at viral suppression predict HCC development in nucleos(t)ide analogue-treated patients with chronic hepatitis B, outperforming HBV core-related antigen (HBcrAg) alone. (Adapted from Kumada et al., Alimentary Pharmacology & Therapeutics, December 2, 2025)
The key finding of the study was that quantifiable HBV RNA levels at the time of achieving undetectable HBV DNA levels were associated with a 3.2-fold increased risk of HCC, independent of traditional risk factors. Kumada adds, “Since HBV is a DNA virus, HBV RNA has not received much attention. Although HBV RNA is produced during the viral replication cycle, we found it quite surprising that it could serve as such a powerful predictor of cancer development.” Specifically, the study indicates that chronic hepatitis B patients with quantifiable HBV RNA levels, particularly those with concurrent liver dysfunction (ALBI grade 2–3), represent a high-risk subgroup warranting intensified surveillance for HCC.
“Our study was conducted at a single center with 311 patients, so the findings need validation,” concludes Kumada. “Our next important step is to confirm these results through multicenter collaborative research. We would greatly appreciate hearing from institutions interested in participating in such collaborative studies.” Such validation would also reveal if the findings hold for other HBV genotypes.
Hidenori Toyoda, Satoshi Yasuda, Yuichi Koshiyama & Takanori Ito at the Ogaki Municipal Hospital; and Tomoyuki Akita & Junko Tanaka at Hiroshima University co-authored the study.
The study was supported by a grant from Roche Diagnostics Japan.
About the study
Journal: Alimentary Pharmacology & Therapeutics
Title: Hepatitis B Virus RNA Predicts Hepatocellular Carcinoma Despite Viral Suppression
Authors: Takashi Kumada, Hidenori Toyoda, Satoshi Yasuda, Yuichi Koshiyama, Takanori Ito, Tomoyuki Akita, Junko Tanaka
DOI: 10.1111/apt.70483
Date: December 2, 2025

 Home
Home














